Case Report - (2021) Volume 16, Issue 1
Osteoporosis during pregnancy â a case report
Astrit M. Gashi1*, Jakup Ismajli1, Idriz Berisha2, Brikene Elshani1, Behar Rraci3 and Adriatik Berisha4Received: 17-Jan-2021 Published: 31-Mar-2021
Abstract
Osteoporosis is a condition that rarely occurs during pregnancy, but due to loss of bone density, bones become fragile and may suffer fractures. During pregnancy, the aetiology of osteoporosis is unknown. But there are a large number of identifiable risk factors that can influence the development of osteoporosis. Generally, symptoms and signs most often begin in the third trimester of the first pregnancy and improve after delivery, as they do not usually recur in subsequent pregnancies. To diagnose osteoporosis, as well as to determine the risk of fractures and follow-up medication are used bone mineral density (BMD) measurement and determination of the level of the final products (biomarkers), which are released during bone degradation and formation. The dual-energy Xray absorptiometry (DEXA) is the leading technique for estimating bone mineral density. So far there is no specific treatment for osteoporosis during pregnancy. In many cases, the adverse effects of osteoporosis are reversible with appropriate and timely intervention. Therefore, treatment with calcium and vitamin D supplements during pregnancy in women who have two or more risk factors for developing osteoporosis may be reasonable.
sushihouse kolstads americanpridefasteners trueforge hotelposeidon youngswoodfinishing arditomason thebestofreno eeclongisland doktervanhecke famsales adla bogatylaw prefplastics kirbycontractinginc unlsp boban dottoressaromolimonica thebestofsanfrancisco vernix digitaldocuments tristatepropertybrokers sotrafib cemcorpny agenziaimmobiliarebuti joesitalianfoodmarket corpoguardiedicitta icsatc antoniniassicurazioni besel strappedincarseatsafety drevobeton blessingconstructionny centre-endorphine qmbtunisia elearning 357 mpress rrappliance ciaautomazioni antikva stubbanvel tacticalpublicrelations mpulshnk paulyboybrand lordshoes ijd-procom thebestrestaurants atkpalvelut ceat leonfukspc pilotexamssa ashgrovecabins universalshielding thebestofcharlotte johnjmazurinc rollnroaster thecabinetwarehouse pocketchangeduo thebestofmilwaukee resan sooli vwe centralwindowcleaning reinforcedplasticslab bugbustersofli ciandrigiardini arfada centrumeigenwijs thebestofmemphis maisonpearly islipll dcgraphicsinc agetranquille relisandroth thebestofcharleston traiteur-wn safi-ingenierie justmyvoice harrishardware louisbarbatolandscaping brightstartoursworld rga-insurance calacatajumper ezantia mrcheapocds van4holiday cigap richtour fagyhatar sicc weshopmall ventovuori sobatrapcapbon unityrubberllc thebestofsaltlakecity ircinc sescoindustries connply storen-servicesenter psnry greatneckcollision ironfitendurance tuscanycountryhouse sansovinocalcio bbradydesign samsam vdtarification springersoil thebestofdayton milantechnology labradoodlesoflongisland daliamohamed theconsultantpowerhouse gunnbrush kruunuosk shulmanproduce balcosupply conso-med federalnetworks bellmoreglass alwaysaffordableconcrete jayteeinsurance carolina-cabins cmorfinance stretchritepackaging dishaairwaysenterprise biocontrol distribio peterivill lcc inspekta jvidesigns royalroseinc calabriapizza fadhila prato-pronto-effetto arbemachine olsonelectricnj tkbl tuttifotokft alpernmd ggsupplywholesale almaxcorporation sotuflex ecustomgutter studenipotok metal-lineconcept rettsodontologi nutecsystems aclotbeach gjonnes-bygg cavalierinternational mnemos southfloridashuttles ajchemicalsupply rachelsfireisland concepto nesponge ultimatestylesofamerica techniquesmadeeasydrivingschool stevesmeatsfreeport eastwest gritbrush plussplan biosens viltkam wikaya paintballconcept justmyvoice securecarkeysupply justmyvoice allcountylegal catt plugandcharge ttandlcontracting justmyvoice islandboatlettering gms-tunisie sportsiena bloeiop touchofclasscollision kotekservice ittoscana pallongislandlacrosse industrialfinishings painoutband rakvag-batforening konemies rrfamilychiropractic infienile shbcgroup footpharmacydirect scuolaguidaprato ans-nettoyage autoskola saafa autolaky1 fixcars longislandelitelandscaping rayscan palaconstruction studio44 crealhome viniferi gavinburke ciprianigiardini davidpokorny osteriailcapodaglio thebestoffairfax centroorafofaccioli ateliervb bbdps thebestoffresno prodigus stratpak umisushirestaurant sotim suldalrenovasjon amer-equip k-kleven jerryspridepotatoes neuroky psicologozampoli jjslandscaping thebestofoklahomacity responsivesales paratie-antiallagamento-shop hearproof cfat ruspinameubles planetbioplastics lynbrook-plumber fcdf-ye brechanparkett valley-stream-plumber diagnosismaker aquavaria jedit garageennour heimdalbygg thebestoflittlerock raybomarine bayshorepaper gmstowing potatura-abbattimento-piante thebestoflouisville michaelalbert thebestofannarbor unitypavers mtnfueloil durub-mudiya lesgensdere dormerking thusney italianvistatravel maiemad gtiuniformcleaning suddenimpactli levituuli sourisalavie mayoiltank mschwartzfeather rands arieslimousines orthoticworld longislandcocktailhours waterjet allislandpaving dukediagnostic klfgoteborg yanezviaggi apruk decogato springeroilltd semapsolar irisgioiellicomprooro msedpsoftware fourcmanagement holemans 7consulting medinet evertile robertwitcomblandscape ceramics adrobotengineering volt-energy huisjacobs chimneyserviceboston eastmainstdental gcbt rememberingbriank elligiardiniespurghi paulslandscaping luisrestorations mgstunisie fixcarsny crcdd hotelprincipessalucca turvahallinta ralphjr thales irrigazione-giardini spantecsystems biomedic fgt-trading sols-egypt spectrumlaboratoriesinc prosecurite spongewarehouse afsainc dellafrancadevelopmentgroup leragazzedifirenze ferrettiwatches dovreentreprenor digitalhvac mostlymica fleurs-velghe autoscuolalebadie interlockingrubbertiles meadowcreekhoa bcn corpjetsupport jrkitchensflooring arteletti
Keywords
osteoporosis; pregnancy; fracture, bone mineral density; DEXA.
Introduction
Bone tissue is a dynamic tissue in a continuous process of destruction and reconstruction. This bone remodelling, otherwise known as bone turnover, allows adaptation to mechanical weight changes and other physical activities. The skeleton consists of two types of bones: [1] cortical bones or compacts, which make up 80 per cent of the total bone mass (mainly the extremities), and [2] trabecular bones or spongy, which make up 20 per cent of the bone mass. Bone formation begins on the outer surface of the cortical bone, while reabsorption occurs on the inner surface [1,2].
In bones, there are three main types of cells involved in the formation and reabsorption of bone tissue such as osteoblasts, osteocytes, and osteoclasts. Together, the three cell types form the osteon or bone modelling unit. Bone remodelling involves the constant resorption of bone by osteoclasts and the regenerative process performed by bone cells called osteoblasts [3].
Bone formation is done by active osteoblasts which synthesize and secrete type I collagen. This process forms the organic matrix called the osteoid, in which calcium and phosphorus are deposited. After complete bone mineralization, osteoblasts lose their osteosynthetic activity and turn into osteocytes. Inside each osteon, channels are found that penetrate the mineralized bone; through these channels, the internal osteocytes maintain the connection with the external osteoblasts. This structure creates great opportunities for the transfer of calcium from the inside out of the osteon and vice versa. The mineralization process necessarily requires a normal concentration of calcium and plasma phosphorus [4].
Alkaline phosphatase and other proteins derived from osteoblasts (such as osteocalcin) participate in this process. The process of bone resorption is not only about the removal of calcium, but through it, the organic matrix is destroyed and consequently, there is a reduction of bone mass. During osteoclast activity, calcium, phosphorus, magnesium, and amino acids such as hydroxyproline and hydroxylysine are released into the extracellular fluid.
Recruitment of osteoblasts and osteoclasts from precursors and the activity of each cell are regulated by various local factors, including lymphokines, cytokines, growth factors, transcription factors, prostaglandins, hormones and calciferol [5,6].
Bone mass is mainly influenced by hereditary and endocrine factors. In particular, endocrine disorders are particularly dangerous during the growth period. The increase in bone length occurs in specialized areas called epiphyseal growth plates. They close at the end of puberty when they have reached the height of an adult. Total bone mass peaks between 25- 35 years old. In this way, the formation and resorption are equalized at the age of 35-45 years, and after this age, bone resorption begins to prevail. In the process of bone circulation, an adult manages to remodel 15 per cent of the total bone mass per year.
Osteoporosis is a disorder in which loss of bone mass or force leads to fractures due to her fragility. So, a characteristic of these bone disorders is the progressive reduction of bone mass and predispose patients to bone fractures. The most common sites of fractures are the spine, femur, and ankles of the feet and hands [7].
The fundamental pathogenetic mechanisms of osteoporosis are [1] failure to form a skeleton with optimal strength during growth and development; [2] rapid and excessive bone resorption resulting in loss of bone mass and disruption of the microarchitecture of bone; and [3] failure to replace lost bone in the new bone, due to defects in bone formation. Many factors play a role in the development of osteoporosis, included here; estrogen deficiency, calcium deficiencies, vitamin D deficiencies, and secondary hyperparathyroidism, etc. Most bone strength is determined by bone mineral density. However, bone strength and risk for fractures are also influenced by other bone qualities such as remodelling rhythm, bone size and geometry, microarchitecture, damage, and matrix qualities.
Most osteoporosis is considered to be polygenic and results from the interaction of common polymorphic alleles with multiple environmental factors. Environmental factors such as weight, physical activity, and calcium intake also affect bone mass in childhood, adolescence, and early adulthood, to a lesser degree than heredity. In some adolescents and young adults, hormonal changes such as anorexia and the use of injectable contraceptives (progestin) can cause a decrease in bone mass.
Osteoporosis can be primary, as well as secondary. Primary osteoporosis is bone loss that occurs during the normal ageing process and menopausal estrogen deficiency. Secondary osteoporosis is defined as bone loss that results from specific clinical disorders and medications. Secondary causes of bone loss include endocrine disorders, disorders of the gastrointestinal or biliary tract (for example; calcium absorption), adverse effects of drug therapy (use of high doses of heparin during pregnancy), immobilization, eating disorders, marrow related disorders, organ transplantation, renal disease, and cancer. But many cases are also idiopathic. Osteoporosis during pregnancy is a rare condition that is characterized by the progressive reduction of bone mass and the predisposition of pregnant women for bone fractures. Most studies have so far failed to provide clear answers about the aetiology of osteoporosis that occurs during pregnancy [8]. Some authors think that a woman starts with a low peak bone mass or other bone diseases, and normal bone loss in pregnancy causes further bone thinning and results in broken bones. Suspected osteoporosis during pregnancy, when the patient presents with severe persistent pain in the back, pelvis, legs, and radiological examination shows signs of osteopenia or osteoporosis. We are presenting one such case, a pregnant woman diagnosed with osteoporosis.
Case Presentation
A 26-year old 1nd gravida with a pregnancy of 34 weeks of gestation comes for an antenatal visit to our clinic and during a routine checkup, she is found to be having complaints of joint pain and inability to gait or move out of bed. Also, there were pedal edema and redness in the joints of the hands and feet. The patient states that the symptoms manifested as severe two weeks ago and that they are constantly aggravated (Fig.1.).
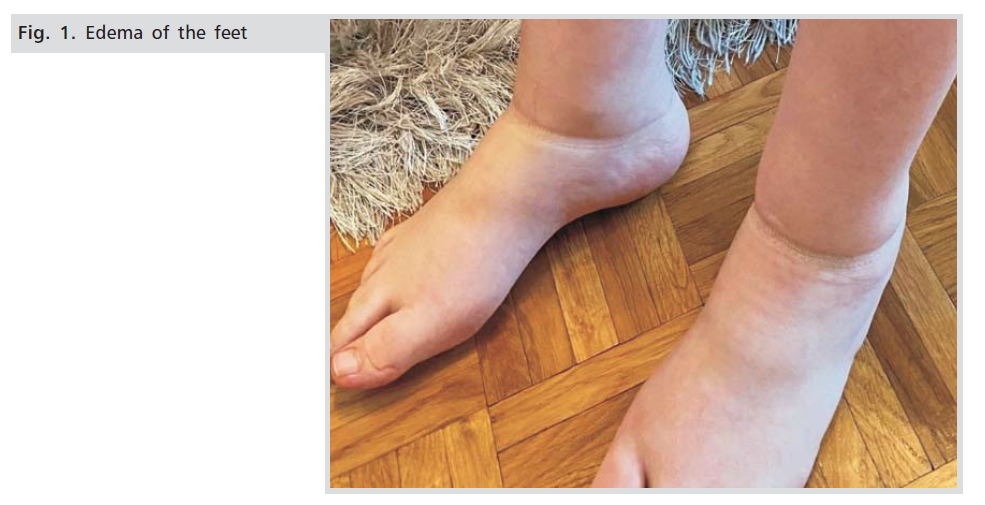
Figure 1: Edema of the feet.
She denies a history of previous cardiac events (arrhythmias, ischemic events, etc.), any history of previous surgery/or intervention, any history of recurrent chest infection, cough, fever, urinary infection, periodontal infection, medication (previous/current). She also denies past histories such as history of tuberculosis, diabetes mellitus, hypertension, osteoporosis, hypercholesterolemia, pulmonary embolus or deep vein thrombosis, blood transfusion, allergy to any drug. Family history is negative for tuberculosis, diabetes mellitus, hypertension, thromboembolic disease, genetic problems, congenital anomalies and any history of congenital heart disease. She denies the use of cigarette smoking, alcohol, and illicit drug use, and domestic violence, and a history of contraceptive practices prior to pregnancy etc. Are excluded and the acute articular syndrome in reactive arthritis, Reiter Syndrome (chlamydial infection), other infectious diseases (yersiniosis), as well as autoimmune diseases (psoriasis, etc.). General physical examination:
It was communicative, time and space-oriented, as well as to the district. Height: 166 cms, weight: 51 kg, body mass index (BMI) = 18.5 kg/m2. She did not have pallor in lower palpebral conjunctiva, dorsum of tongue, teeth, gums and nail beds. Pulse 80 minutes, of regular, and blood pressure - 110 \ 70 mm Hg in right arm supine position. Respiratory rate: 14 per minute. Temperature: 36.8 °C. Pelvic examination: vulva without obvious pathological changes. Vagina of normal length and width, accompanied by light vaginal discharge, odorless and without itching. The cervical dilatation was completely closed, strong and in a central position, and intact amniotic membrane. Ultrasonographic examination: fetal biometric measurements correspond to the 34th week of pregnancy. She had one anterior placement in the placenta with a first degree of maturity. ILA: 15 cm, head presentation, fetal heart rate is regular. Fluximetry in the umbilical artery is normal. It is estimated pelvic adequacy for vaginal delivery.
She was initially suspected of algodystrophy with transient pedal oedema and was assigned for further investigation. Laboratory tests: complete blood count, urinalysis and complete biochemistry were normal. The pain was treated symptomatically (with paracetamol and placement of cold cloths on the leg). Until birth, the patient moved very little, with the help of the assistant. She gave birth in the 39th week of pregnancy, with vaginal delivery, a completely healthy baby. After birth, the patient was called for radiological examinations. Examination was performed by a Hologic QDR device to assess the entire spine, lumbar and lower extremities. Reduction of calcium load in the lumbar spine has been observed, with a T -3.2 score, a value compatible with osteoporosis criteria, according to WHO classification. Also, reduction of calcium load in the hip, with a Tscore of -4.0, a value compatible with osteoporosis, etc. Other bone structures resulted in values that confirmed osteoporosis (Figs.2,3,4). She received standard treatment for osteoporosis, and after 6 weeks, she started walking completely independently.
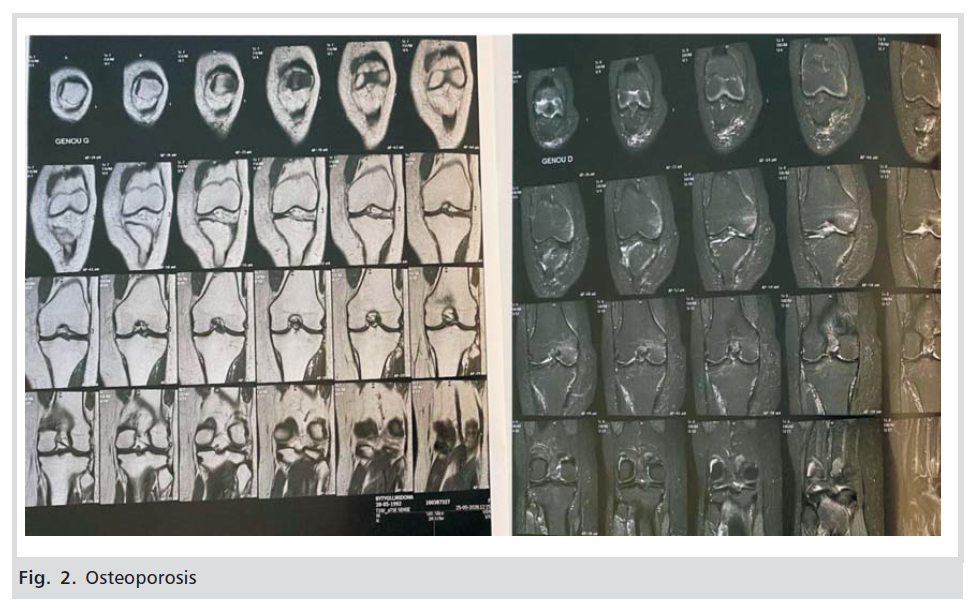
Figure 2: Osteoporosis
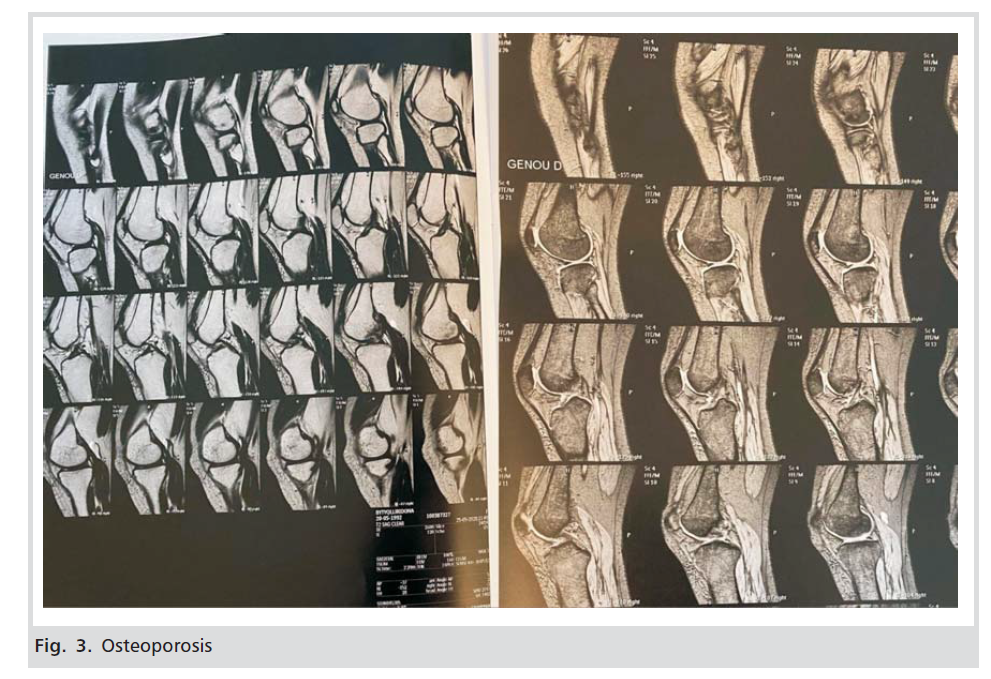
Figure 3: Osteoporosis
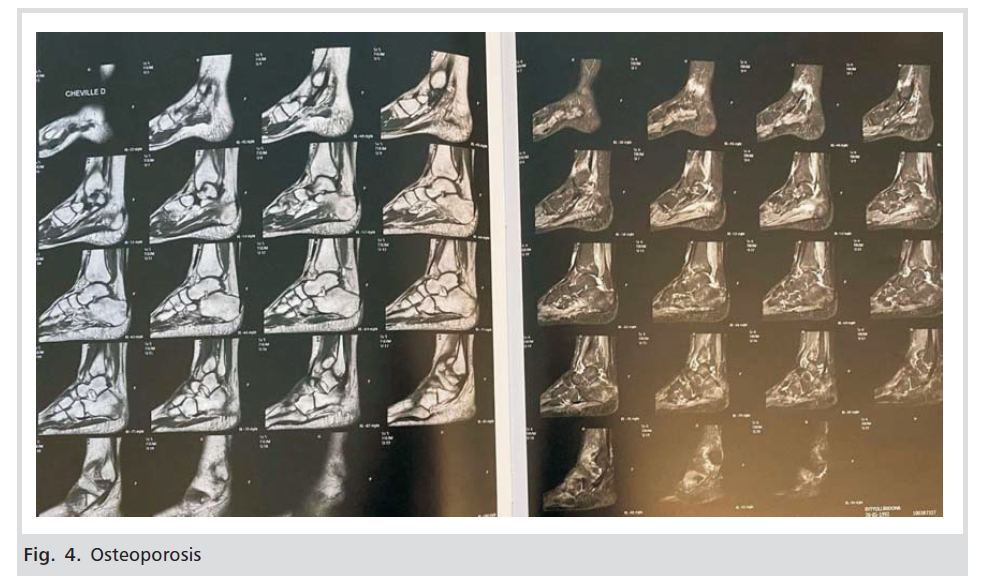
Figure 4: Osteoporosis
Discussion
Osteoporosis during pregnancy is a relatively rare condition. The prevalence, cause and its pathogenesis is unknown. Many factors can affect bone loss during pregnancy and they may have origins; endocrine, vascular, neural, hematological, nutrient-deficiency etc. These risk factors are included in three groups: 1). Immutable factors 2). Variable factors and 3) Factors associated with various pathologies.
In immutable factors are included: age, small stature, early menopause, previous fractures, and a positive family history of osteoporosis. Variable factors include an inadequate intake of calcium and vitamin D in the diet, smoking, excessive alcohol, and caffeine use, sedentary lifestyle, underweight (less than 57 kg) weight loss of more than 10 per cent at age 25 years. Factors associated with medical conditions are hyperthyroidism, hyperparathyroidism, hypercortisolemia, osteomalacia, chronic kidney disease, malabsorption syndrome, hypogonadism, anovulation, rheumatoid arthritis, use of medications such as corticosteroids, usage of GnRH agonist and antagonist, anticonvulsants, and chronic heparin therapy.
Reduced physical activity and lack of calcium or excessive consumption are co-factors in the occurrence of osteoporosis. However, heredity has been assessed as responsible in 50-80% of cases with osteopenia or osteoporosis.
The gestational age at diagnosis of osteoporosis in our study was 34 wks, which was similar to Ofluoglu O, et al. [9]. The patient in our case was primigravida, in the age group 25-35 years, which has also been found in many other studies [9-11]. Classical symptoms of osteoporosis like joint pain, inability to gait, and redness in the joints of the hands, feet and pedal edema were seen in of our case, and other studies have reported the same findings [12-14]. The most common sites of osteoporosis in our case were knees, ankle, and hip, as seen in other articles [15].
In the present case, the patient not had any risk factors, while other studies report the patient had at least one risk factor [10]. Low calcium intake and vitamin D are modestly associated with bone loss, and calcium and vitamin D supplementation protects against bone loss [16-18].
Excessive calcium consumption in some health conditions; for example, during pregnancy we have excessive consumption needed for fetal development. A mother’s low weight is a condition that can result in the loss of bone mass. Excessive physical inactivity or immobility can result in the loss of bone mass [19]. Alcohol consumption, smoking, and corticosteroid use during pregnancy are associated with decreased bone mass and an increased risk of fractures at all ages [20-22].
Initial investigation to diagnose osteoporosis was bone mineral density (BMD) test. Was found a T-score lower than -2.5 standard deviations, which is shown for osteoporosis. Antiosteoporotic treatments with vitamin D 300.000 IU single dose, nasal Calcitonin 400 IU/day, Calcium 1000?mg/day, vitamin D 880 IU/day were initiated.
In healthy bones, bone mineral density (BMD) is expressed as a T-scoring system, which is the number of standard deviations (SD) from the average for a young and healthy woman. A T-score between -1.0 and +2.5 SD is considered normal, a T-score between -1 and -2.5 indicates osteopenia, while a T-score lower than -2.5 indicates osteoporosis for the young adult population (25-35 years old). The term osteopenia is used by radiologists to indicate that radiologically the bone appears to have little mineralization. There is another evaluation index called the Z-score, which shows the standard deviation (SD) between patient measurements and the average bone mass in a patient of the same age and weight. Z-score below -2.5 (below percentile 2.5), requires diagnostic evaluation for secondary osteoporosis.
The dual-energy X-ray absorptiometry (DEXA) is the leading technique for estimating bone mineral density (23, 24 and 25). Early loss of bone mass can be determined by assessing with DEXA, the spine, major trochanter, and neck of the femur, knees, ankle, hip and radius etc.
Generally, for osteoporosis during or after pregnancy, it must be kept in mind during differential diagnosis in patients presenting with lower back pain. The exclusion of other causes for osteoporosis and progressive clinical course are necessary and helpful in the diagnostic process. Early diagnosis and treatment of calcium, vitamin D, and regular follow-up of these cases are particularly very important in the prevention of fractures and increasing the quality of life of the patients.
Conclusion
Osteoporosis is a condition that occurs relatively rarely during pregnancy and clinical features, accompanying metabolic abnormalities, and a physiopathological mechanism has not yet been fully established. During pregnancy, the absorption of calcium in the intestines doubles to meet the fetal demand for calcium, but if the calcium intake is insufficient to meet the needs of the mother and baby, the skeleton of the mother will undergo resorption during the third trimester and progressively immobilizes the mother. Osteoporosis usually occurs in the first pregnancy and does not recur in subsequent pregnancies. This physiological bone resorption does not normally cause fractures. Women who have fractures are more likely to have additional secondary causes of bone loss and fragility. During pregnancy, transient osteoporosis may affect one or both femoral heads, but it also includes localized pedal oedema. Radiographic studies detect loss of bone mass, elevated rates of turnover in the bone, and oedema in the affected portion. Postpartum, a progressive increase in bone mass occurs in most women who present with a fracture during pregnancy, and the need for treatments such as calcitonin, bisphosphonates, strontium ranelate, teriparatide, vertebroplasty, and kyphoplasty are unnecessary. Today, it is possible to diagnose osteoporosis, to evaluate fracture risk, and to reduce that risk with antiresorptive therapies or other available therapies. In many cases, the adverse effects of osteoporosis are reversible with appropriate and timely intervention. Therefore, treatment with calcium and vitamin D supplements during pregnancy in women who have two or more risk factors for developing osteoporosis may be reasonable.
Author´s Contributions
(A) Study Design · (B) Data Collection · (C) Statistical Analysis · (D) Data Interpretation · (E) Manuscript Preparation · (F) Literature Search · (G) Funds Collection
Informed Consent
The patient has provided informed consent for publication of this case report and accompanying images.
Conflict of Interest
The authors declare that there is no financial interest or conflict of interest in this case presentation.
References
- Marks Jr SC, Popoff SN. Bone cell biology: the regulation of development, structure, and function in the ske- leton. Am J Anat. 1988 Sep;183(1):1-44.
- Buckwalter JA, Glimcher MJ, Cooper RR, Recker R. Bone biology. J Bone Joint Surg Am. 1995 Aug 1;77(8):1256- 75.
- Hadjidakis DJ, Androulakis II. Bone remodeling. Annals of the New York Academy of Sciences. 2006 Dec; 1092 (1):385-96.
- Currey JD. The design of mineralised hard tissues for their mechanical functions. Journal of Experimental Biology. 1999 Dec 1; 202(23):3285-94.
- Suda T, Udagawa N, Nakamura I, et al. Modulation of osteoclast differentiation by local factors. Bone. 1995 Aug 1; 17(2):S87-91.
- Eriksen EF. Cellular mechanisms of bone remodeling. Re- views in Endocrine and Metabolic Disorders. 2010 Dec 1;11(4):219-27.
- Court-Brown CM, Caesar B. Epidemiology of adult fractures: a review. Injury. 2006 Aug 1; 37(8):691-7.
- Dunne F, Walters B, Marshall T, Heath DA. Pregnancy associated osteoporosis. Clinical Endocrinology. 1993 Oct; 39(4):487-90.
- Ofluoglu O, Ofluoglu D. A case report: pregnancy-induced severe osteoporosis with eight vertebral fractures. Rheumatology International. 2008 Dec 1; 29(2):197-201.
- Khovidhunkit W, Epstein S. Osteoporosis in pregnancy. Osteoporosis International. 1996 Sep 1; 6(5):345-54.
- Smith R, Winearls CG, Stevenson JC, et al. Osteoporosis of pregnancy. Lancet. 1985 May 25; 325(8439):1178- 80.
- Smith R, Athanasou NA, Ostlere SJ, Vipond SE. Pregnancy associated osteoporosis. QJM: An International Journal of Medicine. 1995 Dec 1; 88(12):865-78.
- Maliha G, Morgan J, Vrahas M. Transient osteoporosis of pregnancy. Injury. 2012 Aug 1; 43(8):1237-41.
- Lose G, Lindholm P. Transient painful osteoporosis of the hip in pregnancy. International Journal of Gynecology & Obstetrics. 1986 Feb; 24(1):13-6.
- Kovacs CS, Ralston SH. Presentation and management of osteoporosis presenting in association with pregnancy or lactation. Osteoporosis International. 2015 Sep 1; 26(9):2223-41.
- Shea B, Wells G, Cranney A, et al. VII. Meta-analysis of calcium supplementation for the prevention of postme- nopausal osteoporosis. Endocr Rev. 2002 Aug; 23(4):552- 9.
- Shea BJ, Adachi JD, Cranney A, et al. Calcium supple- mentation on bone loss in postmenopausal women. Cochrane Database of Systematic Reviews. 2004(1).
- Xu L, McElduff P, D’Este C, Attia J. Does dietary calcium have a protective effect on bone fractures in women? A meta-analysis of observational studies. BJN 2004 Apr; 91(4):625-34.
- Wallace BA, Cumming RG. Systematic review of randomized trials of the effect of exercise on bone mass in pre-and postmenopausal women. Calcified Tissue International. 2000 Jul 1; 67(1):10-8.
- Cauley JA. Public health impact of osteoporosis. Journals of Gerontology Series A: Biomedical Sciences and Medi- cal Sciences. 2013 Oct 1; 68(10):1243-51.
- Bauer DC, Glüer CC, Cauley JA, et al. Broadband ultra- sound attenuation predicts fractures strongly and independently of densitometry in older women: a prospective study. Archives of Internal Medicine. 1997 Mar 24; 157 (6):629-34.
- Cauley JA. Defining ethnic and racial differences in osteoporosis and fragility fractures. Clinical Orthopaedics and Related Research®. 2011 Jul 1; 469(7):1891
- Van der Sluis IM, De Ridder MA, Boot AM, et al. Reference data for bone density and body composition measured with dual energy x ray absorptiometry in white children and young adults. Archives of Disease in Childhood. 2002 Oct 1; 87(4):341-7.
- Hans D, Barthe N, Boutroy S, et al. Pothuaud L, Win- zenrieth R, Krieg MA. Correlations between trabecular bone score, measured using anteroposterior dual-energy X-ray absorptiometry acquisition, and 3-dimensional parameters of bone microarchitecture: an experimental study on human cadaver vertebrae. Journal of Clinical Densitometry. 2011 Jul 1; 14(3):302-12.
- Garg MK, Kharb S. Dual energy X-ray absorptiometry: Pit- falls in measurement and interpretation of bone mineral density. Indian Journal of Endocrinology and Metabolism. 2013 Mar; 17(2):203.
Author Info
Astrit M. Gashi1*, Jakup Ismajli1, Idriz Berisha2, Brikene Elshani1, Behar Rraci3 and Adriatik Berisha42Faculty of Medicine, University of Gjakova Fehmi Agani, Kosovo
3Department of Oncology, Faculty of Medicine, University of Pristine, Pristine, Kosovo
4Department of Hematology, Faculty of Medicine, University of Pristine, Pristine, Kosovo
Copyright:This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.